Kontrola rytmu Vašeho srdce
Kdykoliv, kdekoliv, neomezeně a v naprostém pohodlí
0
+
měření EKG
0
dnů měření
171
+
zachráněných životů
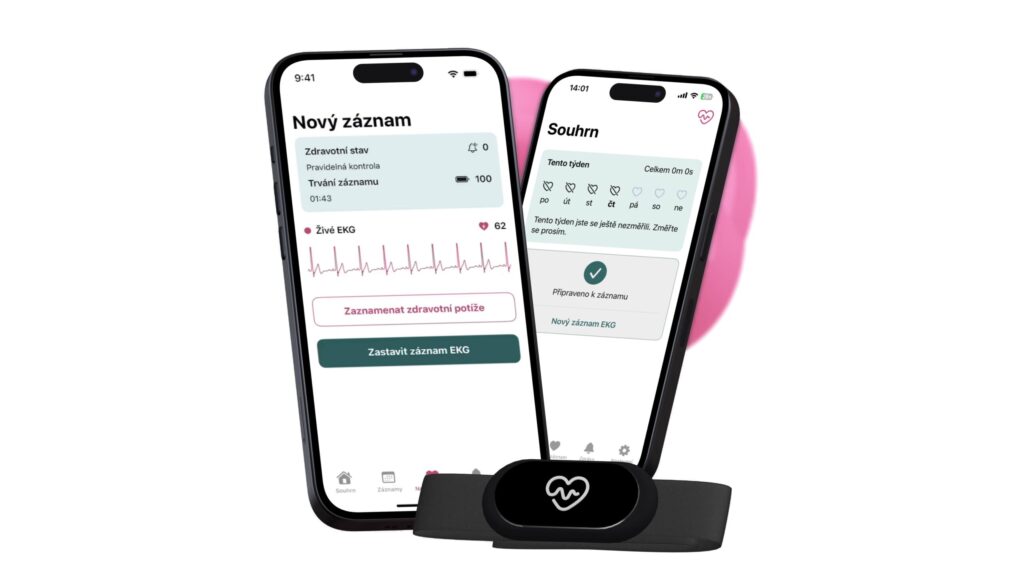
Proč má monitoring srdce smysl?
Kardiovaskulární onemocnění představuje hlavní příčinu úmrtí v České republice. Dlouhodobý monitoring je klíčovým nástrojem prevence, podpory zdraví srdce, včasného rozpoznání a léčby srdečních onemocnění.

Prevence závažných onemocnění
Srdeční arytmie, kterou trpí přes půl milionu lidí v ČR, může vést k srdečnímu selhání, mozkové mrtvici nebo k brzkému nástupu demence. 30 % lidí trpících srdeční arytmií o tom neví, jsou bez obtíží. Můžete být jedním z nich.

Náš životní styl, naše srdce
Jsou v souladu? Zjistěte to! Stres, nedostatek pohybu, obezita, nevyvážená strava, alkohol a kouření srdce výrazně zatěžují. Lepší vědět dříve nežli později.

Řízení rizikových faktorů
Vysoký krevní tlak a cholesterol, cukrovka, dědičnost (i navzdory zdravému životnímu stylu) hrají v neprospěch Vašeho srdce. Monitorujte ho, snižte tak riziko spousty faktorů a dopřejte si klid, protože víte, na čem jste.
Lékařská péče na míru a bez prodlení
Dlouhodobé sledování srdce poskytuje klíčová data pro personalizaci léčby lékařem a doporučení pro zdravý životní styl. Taktéž monitorace uživatelem kdykoliv, zvláště v případě potíží, dokáže urychlit stresující čekání na verdikt, zdali je srdce v pořádku.
Služba Kardi Ai
Služba Kardi Ai propojuje záznamové zařízení EKG v podobě pohodlného hrudního pásu s unikátní aplikací, která je certifikovaná jako zdravotnický prostředek. Aplikace monitoruje rytmus Vašeho srdce a v případě nesrovnalostí Vás okamžitě upozorní. Současně generuje podrobnou zprávu o Vaší srdeční činnosti pro lékaře.
Pravidelné monitorování srdce má smysl. Stačí Vám chytrý telefon, aplikace KARDI AI, hrudní pás a výrazně tak přispějete k prevenci kardiovaskulárních onemocnění, které jsou u nás příčinou 40 % úmrtí. Podchyťte problém dřív, než nastane.
Záznam EKG
Kdykoliv, kdekoliv, neomezeně, za příznivou cenu a ve vysoké kvalitě ověřené kardiology v lékařských studiích.
Vyhodnocení AI
Na základě záznamů EKG umělá inteligence vyhodnocuje činnost srdce a výsledky okamžitě komunikuje přímo uživateli. Pro Vás kýžený klid a jistota, případně upozornění, že je třeba vyhledat lékařskou pomoc. Podrobný report pro lékaře je samozřejmostí.
Propojení s lékařem
KARDI AI přímo propojuje Vaše srdce s kardiologem, který má k Vašim záznamům EKG neustálý přístup. Záznamy jsou umělou inteligencí vyhodnocovány nejen v daný moment, ale i jako celek za týdny, měsíce i roky, a lékaři tak umožní určit přesnější diagnózu, a hlavně ji určit rychleji.
Názory odborníků na Kardi Ai
Jak Kardi Ai přispívá k přesnější a rychlejší diagnostice? Jde o průlomové řešení v péči o srdeční zdraví? Názory a zkušenosti předních lékařů, kteří službě Kardi Ai dali šanci:
„Metodika je obrovským přínosem při záchytu fibrilace síní i v diagnostice paroxysmálních arytmií a nepravidelných palpitací s minimální šancí odhalení při klasické EKG monitoraci. Automatické hodnocení mi umožňuje kdykoliv rychlý přehled o „arytmické“ situaci pacientů, na kterou můžu ihned reagovat. Díky snadné spolupráci se také významně posiluje důvěrný vztah s pacienty.“
doc. MUDr. Ivo Oral, CSc.
Olomouc, Česká republika

„Kardi Ai jsem si oblíbila hlavně pro rychlou dostupnost v případě potíží a možnost záchytu arytmií, které se nám nedaří detekovat při běžně dostupných monitoracích.
Díky tomu jsme schopni po domluvě s pacientem rychle nabídnout optimální léčbu, ale také vyloučit arytmogenní příčinu jiných obtíží.“
MUDr. Zdeňka Pospíšilová
Brno, Česká republika

„Kardi Ai ráda využívám u svých pacientů s nejasnými palpitacemi. U 30 % z nich byla nalezena paroxysmální fibrilace síní, která indikovala provedení radiofrekvenční ablace. Těším se spolupráci do budoucna a zejména možnost detekce i jiných forem srdečních arytmií.“
MUDr. Pavla Gablasová, Ph.D.
Brno, Česká republika

